In every age, our bodies need to adapt to new challenges. Apparently, in this age, we need to solve another problem induced by texting, “Text Neck.”
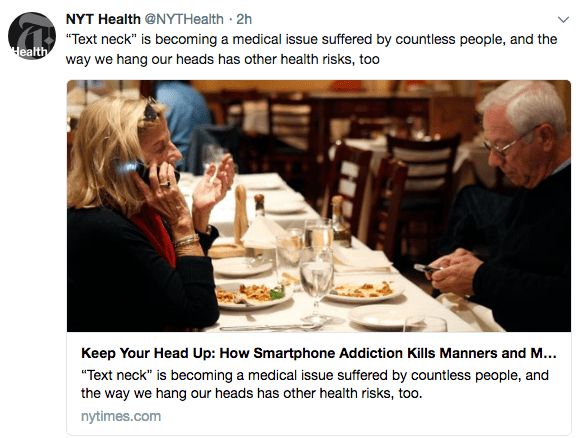
NY Times: Keep Your Head Up: How Smartphone Addiction Kills Manners and Moods
Here’s an excerpt:
The average human head weighs between 10 and 12 pounds, and when we bend our neck to text or check Facebook, the gravitational pull on our head and the stress on our neck increases to as much as 60 pounds of pressure. That common position, pervasive among everyone from paupers to presidents, leads to incremental loss of the curve of the cervical spine. “Text neck” is becoming a medical issue that countless people suffer from, and the way we hang our heads has other health risks, too, according to a report published last year in The Spine Journal.
Posture has been proven to affect mood, behavior and memory, and frequent slouching can make us depressed…
And the remedy can be ridiculously simple: Just sit up.
My take: Smartphone use increases the risk of many health problems besides “Text Neck” including car accidents. Their use also contributes to missing social cues, including placing those in front of you behind those who interrupt conversations with texts and phone calls.