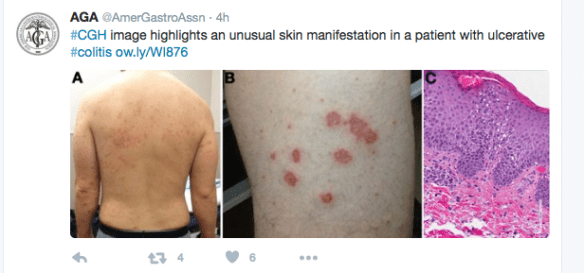
As noted in previous blog posts (see below), anti-tumor necrosis factor (anti-TNF) therapy has been associated with skin problems. The following study/abstract elaborate on this issue further and indicate that while ~30% of patients with IBD may develop skin reactions, only 28 of 917 (3%) patients required anti-TNF therapy to be discontinued due to skin reactions.
I Cleynen et al. Ann Intern Med. Published online 8 December 2015 doi:10.7326/M15-0729 Characteristics of Skin Lesions Associated With Anti–Tumor Necrosis Factor Therapy in Patients With Inflammatory Bowel Disease: A Cohort Study ONLINE FIRST
Objective: To describe patients treated with anti-TNF antibodies who did and did not develop skin lesions.
Design: Retrospective cohort.
Setting: Single IBD tertiary referral center.
Patients: 917 consecutive patients with IBD who initiated anti-TNF therapy.
Measurements: Skin lesions, patient demographic characteristics, treatments, clinical course, and serologic and genetic markers.
Results: During a median follow-up of 3.5 years (interquartile range [IQR], 0.5 to 7.4 years), skin lesions associated with the use of anti-TNF therapy developed in 264 of 917 (29%) patients (psoriasiform eczema, 30.6%; eczema, 23.5%; xerosis cutis, 10.6%; palmoplantar pustulosis, 5.3%; psoriasis, 3.8%; other, 26.1%). Lesions typically developed at flexural regions, genitalia, and the scalp, especially the psoriasiform lesions. Thirty-one percent of women and 26% of men developed lesions. Median cumulative doses (2864 mg/y [IQR, 2203 to 3819 mg/y] and 2927 mg/y [IQR, 2377 to 3667 mg/y]) and trough levels (4.2 µg/mL [IQR, 2.6 to 5.8 µg/mL] and 4.0 µg/mL [IQR, 1.6 to 5.9 µg/mL]) of infliximab were similar in patients with and without lesions. All but 28 patients (11%) were successfully managed without needing to stop therapy because of lesions.
Limitation: Retrospective nature and no matched control group of patients not receiving anti-TNF therapy.
Conclusion: Skin lesions occur frequently in association with anti-TNF therapy but rarely require discontinuation of therapy. Close surveillance and early referral to a dedicated dermatologist are recommended.
Related blog posts: