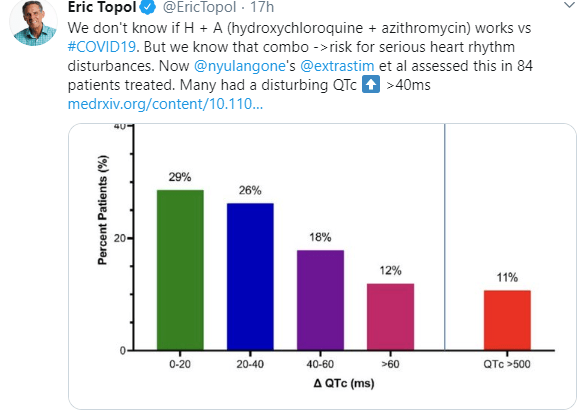
Here’s a commentary explaining why hydroxychloroquine is NOT proven effective:
Annals of Internal Medicine -Link: A Rush to Judgment? Rapid Reporting and Dissemination of Results and Its Consequences Regarding the Use of Hydroxychloroquine for COVID-19
Some of the key points:
- While the study suggested more rapid clearance of SARS-CoV-2 virus at day 6 in those treated with hydroxychloroquine/azathioprine (n=20), the authors excluded 6 from the treatment group including one patient who died and three who were transferrred to the ICU. In addition, the treatment group had a lower viral load at the start of treatment.
- Other viral infections, including influenza, have also had in vitro data suggesting efficacy with hydroxychloroquine but this did not translate into clinical efficacy in clinical trials.
- “The hydroxychloroquine shortage not only will limit availability to patients with COVID-19 if efficacy is truly established but also represents a real risk to patients with rheumatic diseases who depend on HCQ for their survival.”
————————–
A Di Giorgio et al (J Pediatr 2020; 218: 121-9) provide long-term data (median f/u of 14.5 years) from a retrospective review on 83 children with autoimmune hepatitis (AIH, n=54)/autoimmune sclerosing cholangitis (ASC, n=29). Median age at presentation, between 2000-2004 was 12.1 years
Key findings:
- 29% had histologic evidence of cirrhosis at diagnosis
- At a median followup of 14.5 years, 99% were alive, 11 underwent transplantation. In those who underwent transplantation, 5-year and 10-year survival was 95% and 88% respectively.
- ASC was associated with IBD in 73% of cases, compared to 33% of AIH patients.
- Treatment: 95% of all patients had normalization with transaminases with immunosuppressive treatment (most commonly azathioprine with prednisone 2.5-5 mg/day). ASC patients also received ursodeoxycholic acid 15-20 mg/kg/day.
- Immunologic remission: 47% achieved immunologic remission which required normal IgG levels and negative/low ANA/SMA <1:20 in addition to normal transaminases.
- Liver transplantation was needed in 28% of ASC compared to 9% of AIH patients; overall, 83% experienced 15-year transplant-free survival. Median age of those needing a liver transplant was 19.3 years.
- Immunosuppression withdrawal was attempted in 12 patients after a median of 4.5 years of treatment. 9 were able to stay off immunosuppression.
- An increase in case frequency was noted during the last 4 decades at this center, from 3.6 cases/year to 5.4 case/year.
- Four patients had isolated infrequent autoantibodies of anti-SLA (n=3) nad antiLC-1 (n=1). SLA =liver soluble antigen, LC-1 =liver cytosol antibody type 1. Thus, in those with suspected AIH/ASC, testing for these autoantibodies is important in ~5%.
- Pathology: 18% did not have classical features of interface hepatitis. Instead, some had lymphocytic/lymphoplasmocytic infiltrate without spillover into the parenchyma.
- Progression from AIH to ASC occurred in 3 patients on followup cholangiography.
- ASC would have been overlooked in 41% if one relied on pathology alone -reaffirming need for biliary imaging.
My take: This article has a number of useful points and with an overarching message that long-term outcomes are good for children with AIH/ASC.
Related blog posts:
B Freiberg et al. 2020; 218: 221-31. This grand rounds describes the extensive workup of a 12 year old with splenomegaly ultimately due to splenic vein stenosis. The report provides a nice review of hepatologic, hematologic, infectious, and other causes of splenomegaly as well as a work-up algorithm. (look for everything).
Initial evaluation per algorithm should start with CBC/d, retic, blood smear, liver biochemistries, GGT, coags, EBV VCA IgM, CMV IgM, Parvovirus IgM, and complete abdominal ultrasound with doppler.
Hepatologic causes of splenomegaly include the following:
- cirrhosis with portal hypertension
- autoimmune hepatitis/autoimmune sclerosing cholangitis
- congenital hepatic fibrosis
- hepatoportal sclerosis
- nodular regenerative hyperplasia
- storage disease and inborn errors of metabolism which includes lipidosis (Gaucher, Niemann-Pick), mucopolysaccharidoses, defects in carbohydrate metabolism (galactosemis, hereditary fructose intolerance), sea-blue histiocyte syndrome
- anatomic disorders: portal/splenic thrombosis, Budd-Chiari, cysts, hamartomas, hemangiomas, hematoma, peliosis
Other causes of splenomegaly: infecions, hematologic-oncologic, and rheumatic disorders
Related blog posts:

| The U.S. Food and Drug Administration today announced it is requesting manufacturers withdraw all prescription and over-the-counter (OTC) ranitidine drugs from the market immediately. This is the latest step in an ongoing investigation of a contaminant known as N-Nitrosodimethylamine (NDMA) in ranitidine medications (commonly known by the brand name Zantac). The agency has determined that the impurity in some ranitidine products increases over time and when stored at higher than room temperatures and may result in consumer exposure to unacceptable levels of this impurity. As a result of this immediate market withdrawal request, ranitidine products will not be available for new or existing prescriptions or OTC use in the U.S.
New FDA testing and evaluation prompted by information from third-party laboratories confirmed that NDMA levels increase in ranitidine even under normal storage conditions, and NDMA has been found to increase significantly in samples stored at higher temperatures, including temperatures the product may be exposed to during distribution and handling by consumers. The testing also showed that the older a ranitidine product is, or the longer the length of time since it was manufactured, the greater the level of NDMA. These conditions may raise the level of NDMA in the ranitidine product above the acceptable daily intake limit. |