I Kaji et al. Gastroenterol 2020; 159: 1390-1405. Full free text: Lysophosphatidic Acid Increases Maturation of Brush Borders and SGLT1 Activity in MYO5B-deficient Mice, a Model of Microvillus Inclusion Disease
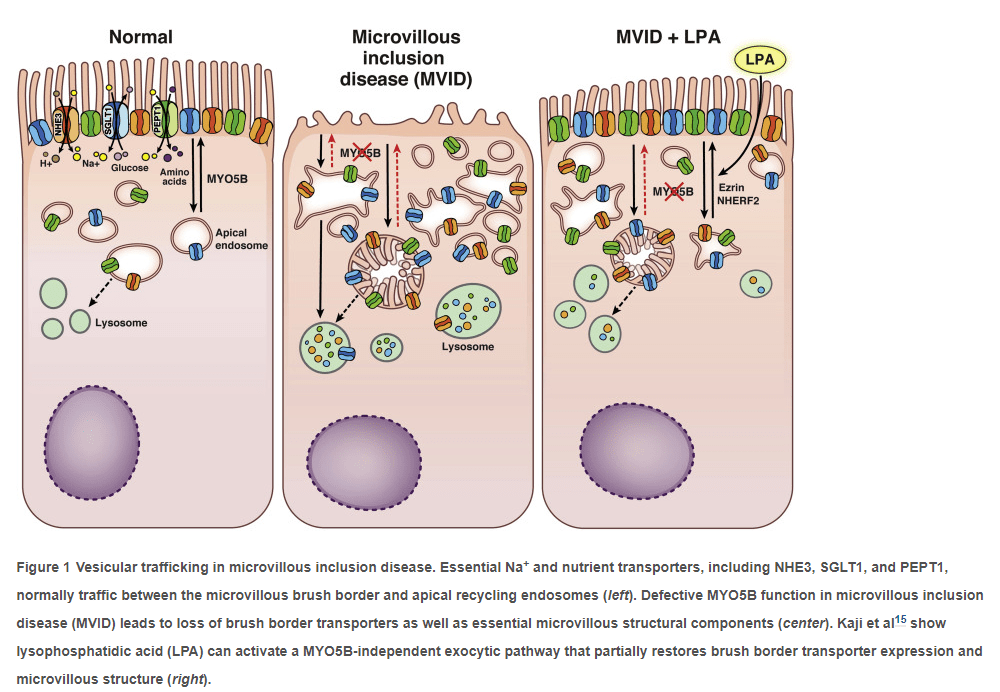
Key finding: Lysophosphatidic acid (LPA)partially restored the brush border height and the localization of SGLT1 and NHE3 in small intestine of MYO5B-knockout mice and enteroids. There are a number of high quality figures that illustrate these effects:

Editorial, S Abtahi, JR Turner. Gastroenterol 2020; 159:1233-1235: Full free text: Exploiting Alternative Brush Border Trafficking Routes to Treat Microvillous Inclusion Disease
Background (from editorial):
- Small bowel biopsies in MVID include enterocytes that have either sparse, blunted microvilli or lack microvilli completely. Large cytoplasmic inclusions with prominent luminal microvilli are, however, present along with increased numbers of subapical lysosomes and other small vesicles
- Biochemically, brush border expression of the Na+-glucose cotransporter SGLT1 (Slc5a1), the N+-H+ exchanger NHE3 (Slc9a3), and aquaporin 7 are markedly decreased in patients with MVID
- Myo5b knockout in mice induces histopathologic and clinical features of MVID, including villous blunting, growth failure, and increased stool water, that is, diarrhea
- Previous studies have shown that NHE3 trafficking from the apical storage pool to the brush border could be triggered by lysophosphatidic acid (LPA)
Key points from editorial
- Kaji et al treated adult Myo5bf/f x vil-CreERT2 mice with …oral or systemic LPA administration. Villous blunting, microvillous loss, and apical lysosomal expansion were substantially reversed after 4 days of systemic LPA treatment
- Although the morphologic and physiologic responses induced by LPA are striking, the weight loss that began within 2 days of Myo5b knockout was not attenuated. Thus, despite being remarkably beneficial when assessed using laboratory assays, LPA has not yet been shown to be an effective therapeutic agent.
My take (borrowed from editorial): This study shows “there are multiple trafficking pathways to the brush border and that one of these can be exploited to overcome defects in another.”