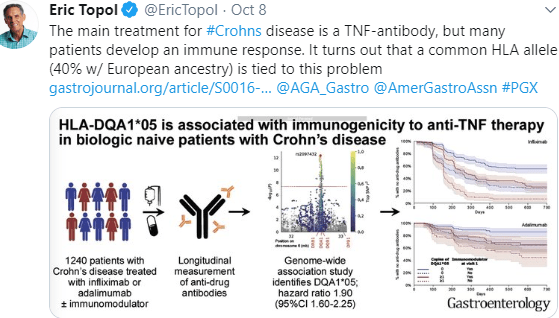
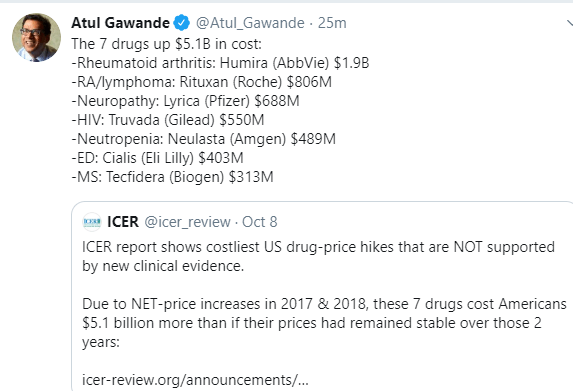A recent opinion piece from FoodSafetyNews highlights the lack of transparency from the FDA regarding food-borne outbreaks (several more listed below).
Bill Marler: Publisher’s Platform: A bit more about the FDA and lack of Transparency
Here’s an excerpt:
The Halloween disclosure of a multistate E. coli outbreak linked to romaine lettuce raises another concern about the FDA and transparency — the failure to disclose where consumers purchased the tainted product..
Under the Freedom of Information Act and Title 21 of the Code of Regulations, government agencies — and specifically, the FDA — are told to exempt trade secrets and commercial information from any of their releases…
Formulations, ingredients and how products are made are trade secrets. Who supplied the tainted raw material, who made the tainted product and where the tainted product was sold are not a trade secrets – especially during an outbreak. Simplicity, transparency and consistency allows for a visible supply chain and one that consumers can have confidence in.
Recent outbreaks (thanks to colleague for these references):
Multistate Salmonella Outbreak Linked To Ground Beef Causes One Death, Eight Hospitalizations
- Reuters (11/1, Maddipatla) reported, “A multistate outbreak of salmonella linked to ground beef has caused one death in California and eight hospitalizations, U.S. health officials said on Friday. A total of 10 people in six U.S. states were infected with a strain of the bacteria called Salmonella Dublin, according to the Centers for Disease Control and Prevention.”
- TIME (11/2, Carlisle) reported, “Officials have not yet identified a single common source of the ground beef that is believed to be spreading the Salmonella Dublin based on epidemiological and laboratory evidence. According to the CDC, the sick individuals reported eating different brands of ground beef at different locations.”
- CNN (11/1, Christensen) also reported the story.
Previously Undisclosed E. Coli Outbreak Linked To Romaine Lettuce Sickened Nearly Two Dozen People, FDA Says
- The Washington Post (11/1, Brice-Saddler) reported, “A previously undisclosed E. coli outbreak linked to romaine lettuce sickened nearly two dozen people between July and early September, the Food and Drug Administration said Thursday – a delayed announcement one food safety lawyer called a ‘lie to the public in all respects.’” The piece added, “Illnesses associated with the outbreak infected 23 people across 12 states from July 12 to Sept. 8, according to the FDA. No patients died of their illnesses, and officials say there is no ongoing public health risk.”
Dozens more fresh vegetable products because of Listeria monocytogenes risk (11/4) (FoodSafetyNews.com)
- A (Canadian) nationwide recall of freshcut vegetables continues to expand with dozens of products and multiple brands now on the list. Products potentially contaminated with Listeria monocytogenes are cole slaw, riced cauliflower, green beans, noodles, kale salads and more. Some of the products do not expire for 10 days or more, so consumers and businesses are urged to check their supplies for the recalled products listed here by the Canadian government
My take: Food-borne illnesses cause 48 million cases in U.S. each year (CDC estimates) and 3000 deaths (MMWR 64:2, 2015). More transparency is needed.
Related blog post: Food Safety Lecture-It’s Still A Jungle Out There