JB McCannon et al. NEJM 2023; 389: 1902-1911. Case 35-2023: A 38-Year-Old Woman with Waxing and Waning Pulmonary Nodules
In this case report, A 38-year-old woman was evaluated because of dyspnea, chest discomfort, and waxing and waning pulmonary nodules. She had a prior history of ulcerative colitis. This article reviews reasons for pulmonary nodules including cancer, infection, vasculitis, connective tissue disorders, sarcoidosis and inflammatory bowel disease (IBD) which has a number of pulmonary manifestations including necrobiotic nodules.
In this case, the granulomatous lung disease was attributed to be an extraintestinal manifestation of IBD. She was treated with TNF-alpha targeted therapy which has been effective in a prior case report (J Crohns Colitis 202; 14: 480-489).
My first reaction to this article — I have seen this! However, our case was atypical in that the 15 year old patient presented with respiratory symptoms (no preceding GI diagnosis). It was noted that her gastric wall was severely thickened as an incidental finding on her chest CT which showed extensive tiny pulmonary nodules. Her endoscopy showed disease isolated to her stomach. Both her gastric findings and CT of her chest resolved with infliximab treatment. This included mucosal healing of her stomach on followup endoscopy.
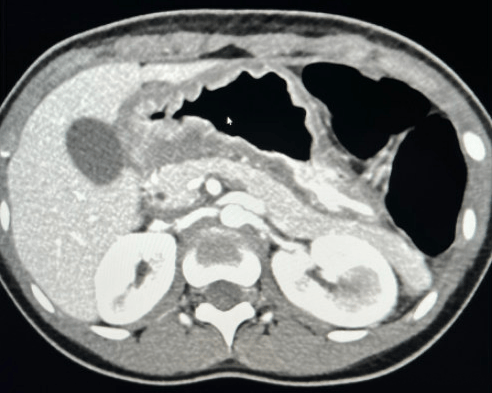
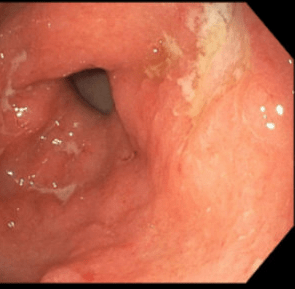
Related blog post: IBD Update January 2015 (Part 1) NEJM 2014; 371: 2418-27 -case report of 9 yo with Crohn’s Disease and pulmonary nodules