N Nguyen , M Bauer. JPGN Rep. 2026;1-3. Successful treatment of eosinophilic esophagitis with upadacitinib prescribed for atopic dermatitis. doi:10.1002/jpr3.70170
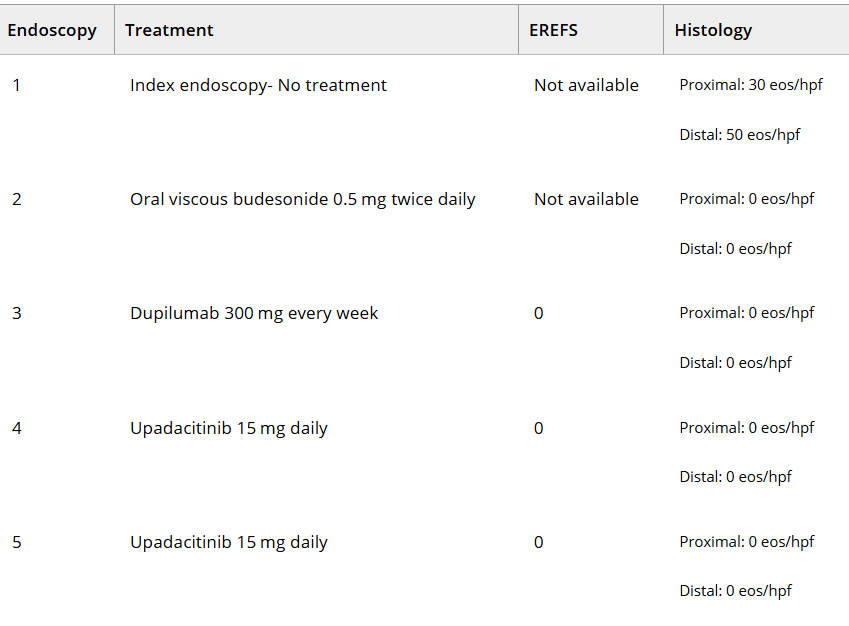
This case report describes a 15 yo with severe atopic dermatitis and multiple atopic diseases whose eosinophilic esophagitis remained in remission after starting upadacitinib, a JAK1 inhibitor, and stopping dupilumab. JAK1 inhibitors, such as upadacitinib and abrocitinib, are approved for severe AD.
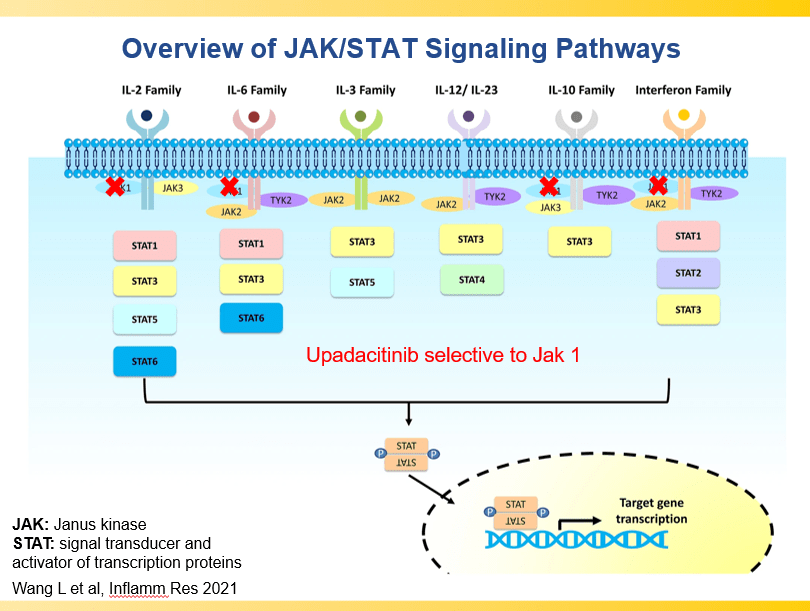
The discussion notes that there had been a prior case report of tofacitinib, a JAK1/JAK3 inhibitor, effectively treating refractory EoE. The authors “hypothesize that JAK inhibition of key Th1 and Th2 signaling pathways including IL-4, IL-13, and TSLP could effectively treat EoE, while also treating AD.”
My take (borrowed from authors): “If upadacitinib is used for the treatment of AD, cessation of other therapies for EoE, particularly biologics like dupilumab, should be strongly considered.”
Related blog posts:
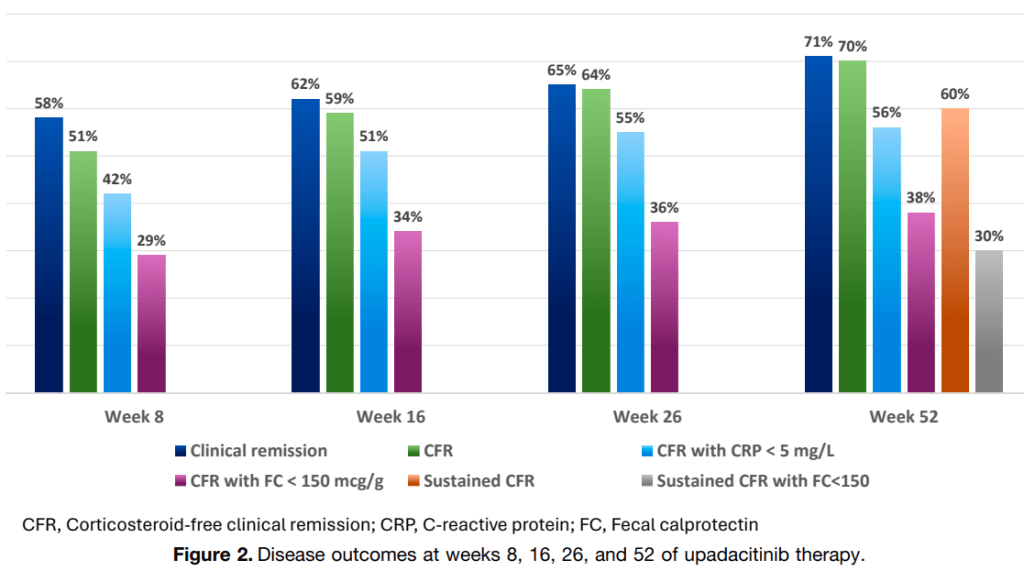
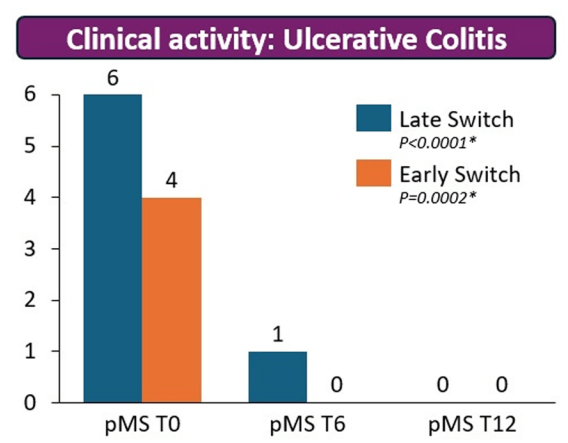
- Upadacitinib for Pediatric Ulcerative Colitis
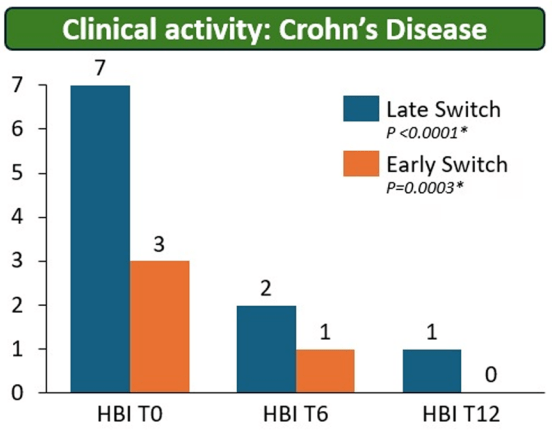
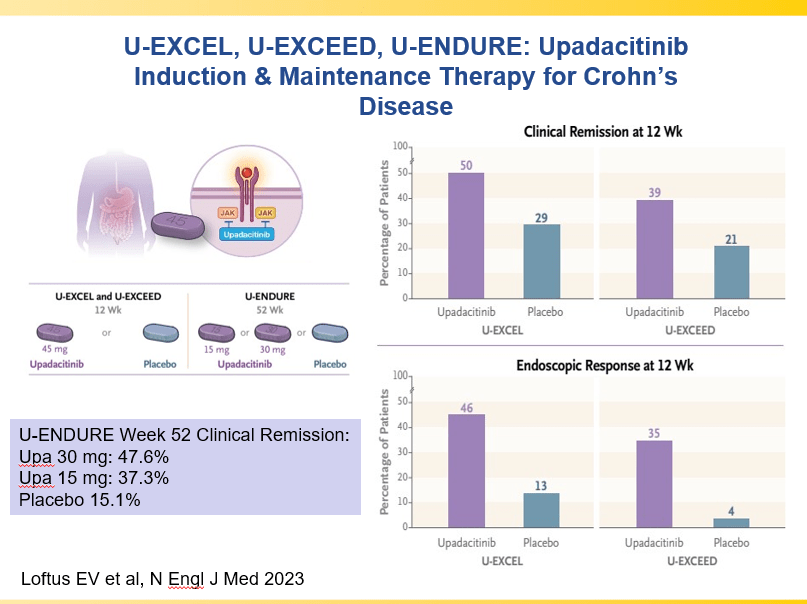
- Upadacitinib for Crohn’s Disease: U-ENDURE Study
- “Real-World” Experience: High Dose Upadacitinib Recaptures IBD Response
- Long-term Efficacy and Safety of Upadacitinib for Ulcerative Colitis
- Upadacitinib’s Effectiveness for Perianal Fistulizing Crohn’s Disease
- Drug Therapy for Celiac Disease: Case Report (Tofacitinib) Another beneficial off-target effect
- Dupilumab (Dupixent) for Young Children with Eosinophilic Esophagitis (Published Data)
- “Real-World” Dupilumab for Eosinophilic Esophagitis
- When to Use Dupilumab for Eosinophilic Esophagitis: Multispecialty Guidelines
- Dupixent Approved in Younger Children (15 kg+) (Dupixent dosing)
- Dupilumab for FPIES