
About gutsandgrowth
I am a pediatric gastroenterologist at GI Care for Kids (previously called CCDHC) in Atlanta, Georgia. The goal of my blog is to share some of my reading in my field more broadly. In addition, I wanted to provide my voice to a wide range of topics that often have inaccurate or incomplete information.
Before starting this blog in 2011, I would tear out articles from journals and/or keep notes in a palm pilot. This blog helps provide an updated source of information that is easy to access and search, along with links to useful multimedia sources.
I was born and raised in Chattanooga. After graduating from the University of Virginia, I attended Baylor College of Medicine. I completed residency and fellowship training at the University of Cincinnati at the Children’s Hospital Medical Center. I received funding from the National Institutes of Health for molecular biology research of the gastrointestinal tract.
During my fellowship, I had the opportunity to work with some of the most amazing pediatric gastroenterologists and mentors. Some of these individuals included Mitchell Cohen, William Balistreri, James Heubi, Jorge Bezerra, Colin Rudolph, John Bucuvalas, and Michael Farrell. I am grateful for their teaching and their friendship. During my training with their help, I received a nationwide award for the best research by a GI fellow.
I have authored numerous publications/presentations including original research, case reports, review articles, and textbook chapters on various pediatric gastrointestinal problems. In addition, I have been recognized by Atlanta Magazine as a "Top Doctor" in my field multiple times.
Currently, I am the vice chair of the section of nutrition for the Georgia Chapter of the American Academy of Pediatrics. In addition, I am an adjunct Associate Clinical Professor of Pediatrics at Emory University School of Medicine. Other society memberships have included the North American Society for Pediatric Gastroenterology Hepatology and Nutrition (NASPGHAN), American Academy of Pediatrics, the Food Allergy Network, the American Gastroenterology Association, the American Association for the Study of Liver Diseases, and the Crohn’s and Colitis Foundation.
As part of a national pediatric GI organization called NASPGHAN (and its affiliated website GIKids), I have helped develop educational materials on a wide-range of gastrointestinal and liver diseases which are used across the country. Also, I have been an invited speaker for national campaigns to improve the evaluation and treatment of gastroesophageal reflux disease, celiac disease, eosinophilic esophagitis, hepatitis C, and inflammatory bowel disease (IBD). Some information on these topics has been posted at my work website, www.gicareforkids.com, which has links to multiple other useful resources.
I am fortunate to work at GI Care For Kids. Our group has 17 terrific physicians with a wide range of subspecialization, including liver diseases, feeding disorders, eosinophilic diseases, inflammatory bowel disease, cystic fibrosis, DiGeorge/22q, celiac disease, and motility disorders. Many of our physicians are recognized nationally for their achievements. Our group of physicians have worked closely together for many years. None of the physicians in our group have ever left to join other groups. I have also worked with the same nurse (Bernadette) since I moved to Atlanta in 1997.
For many families, more practical matters about our office include the following:
– 14 office/satellite locations
– physicians who speak Spanish
– cutting edge research
– on-site nutritionists
– on-site psychology support for abdominal pain and feeding disorders
– participation in ImproveCareNow to better the outcomes for children with inflammatory bowel disease
– office endoscopy suite (lower costs and easier scheduling)
– office infusion center (lower costs and easier for families)
– easy access to nursing advice (each physician has at least one nurse)
I am married and have two sons (both adults). I like to read, walk/hike, bike, swim, and play tennis with my free time.
I do not have any financial relationships with pharmaceutical companies or other financial relationships to disclose. I have helped enroll patients in industry-sponsored research studies.
A recent multicenter case-controlled study (MJ Siegel, J Freeman, W Ye et al. J Pediatr 2020; 219: 62-9) show that ultrasonography can identify children with cystic fibrosis (CF) at increased risk for developing advanced CF liver disease; it is well-recognized that currently advanced CF liver disease occurs predominantly in children.
Among 722 participants who underwent ultrasonography as part of a planned 9 year research study, 65 had heterogeneous liver pattern and 592 had a normal liver pattern at baseline.
Key findings at planned 4-year interim analysis in a subgroup of 55 with (baseline) heterogeneous liver pattern and 116 with (baseline) normal liver pattern:
- Those with heterogeneous liver pattern had higher median biochemical markers of liver disease: ALT 42 vs 32, GGT 36 vs 15, AST to platelet ratio index: 0.7 vs 0.4
- Those with heterogeneous liver pattern were at ~9-fold increased risk of developing a nodular liver pattern (23% vs. 2.6%).
- The authors did not identify specific clinical risk factors that predict the development of nodular liver ultrasound pattern
My take: Even among those with a heterogeneous pattern, the majority will not develop a ultrasonography (nodular) pattern of advanced liver disease. Much more insight in this area is needed with the advancement in medical treatments and with the more availability of elastography.
Related blog posts:

Island Ford Nat’l Recreation Area/Chattahoochee River
NEJM: Children with Covid-19 in Pediatric Emergency Departments in Italy
Key points:
- Children younger than 18 years of age who had Covid-19 composed only 1% of the total number of patients; 11% of these children were hospitalized, and none died
- The Coronavirus Infection in Pediatric Emergency Departments (CONFIDENCE) study involved a cohort of 100 Italian children younger than 18 years of age with Covid-19 (median age 3.3 years)
- .Common symptoms were cough (in 44% of the patients) and no feeding or difficulty feeding (in 23%) (especially if <2 years)
- Fever, cough, or shortness of breath occurred in 28 of 54 of febrile patients (52%)
- Of the 9 patients who received respiratory support, 6 had coexisting conditions
My take: This study provides additional data indicating that severe outcomes are rare in children with Covid-19.
Related article from NY Times: How Coronavirus Mutates and Spreads
An excerpt:
Researchers have found that the coronavirus is mutating relatively slowly compared to some other RNA viruses, in part because virus proteins acting as proofreaders are able to fix some mistakes. Each month, a lineage of coronaviruses might acquire only two single-letter mutations.
In the future, the coronavirus may pick up some mutations that help it evade our immune systems. But the slow mutation rate of the coronavirus means that these changes will emerge over the course of years.
That bodes well for vaccines currently in development for Covid-19. If people get vaccinated in 2021 against the new coronavirus, they may well enjoy a protection that lasts for years.
Related blog posts:


A piece of good news: —Doubletree Reveals Cookie Recipe
This blog does not receive any sponsorships. That being said, my wife made a batch of these cookies and they are delicious! My advice is to freeze half the batch and cook some later to avoid overconsumption.

A recent commentary (ECF Brown. NEJM 2020; 382: 1189-91) helps explain why surprise billing still exists despite bipartisan contempt.
Key points:
- “An estimated 20% of U.S. emergency-department visits, 9% of inpatient admissions, and more than half of ambulance or air-ambulance transports involve an out-of-network provider.”
- “Surprise medical billing…is more prevalent …in groups owned by certain private-equity investment companies.”
- There are generally two approaches to solving the problem of surprise medical billing, either arbitration or using a payment benchmark, the former generally favors providers and the latter generally favors payers.
- “Deep-pocketed private equity firms continue to oppose any legislation that cuts into their profits, as they increase their investments in physician practices…Nearly everyone else agrees that patients should be protected from surprise medical bills.”
My take (borrowed from the author): The outcome of the surprise medical billing issue “raises questions about both the role of private equity in health care and the ability of Congress to pass meaningful health care legislation.”
Related blog posts:

Blood Mountain Trail
Full Text: JD Feuerstein et al. Gastroenterol 2020; 158: 1450-61. AGA Clinical Practice Guidelines on the Management of Moderate to Severe Ulcerative Colitis
Full Tex PDF: AGA Clinical Practice Guidelines on the Management of Moderate to Severe Ulcerative Colitis


Associated articles included the following:
- Clinical decision support tool (1462-63)
- PDF: Spotlight (summary -images above) (1464)
- Technical Review (1465-96)
Key recommendations:
- 2a. In adult outpatients with moderate to severe UC who are naïve to biologic agents, the AGA suggests using infliximab or vedolizumab rather than adalimumab, for induction of remission. Comment: Patients, particularly those with less severe disease, who place higher value on the convenience of self-administered subcutaneous injection, and a lower value on the relative efficacy of medications, may reasonably chose adalimumab as an alternative
- 2c. In adult outpatients with moderate to severe UC who have previously been exposed to infliximab, particularly those with primary nonresponse, the AGA suggests using ustekinumab or tofacitinib rather than vedolizumab or adalimumab for induction of remission.
- 6. In adult outpatients with moderate to severe UC, the AGA suggests early use of biologic agents with or without immunomodulator therapy rather than gradual step up after failure of 5-ASA. Comment: Patients, particularly those with less severe disease, who place higher value on the safety of 5-ASA therapy and lower value on the efficacy of biologic agents or tofacitinib may reasonably chose gradual step therapy with 5-ASA therapy.
- 10. In hospitalized adult patients with ASUC refractory to intravenous corticosteroids, the AGA suggests using infliximab or cyclosporine
Summary of recommendations:

Related blog posts:
Disclaimer: This blog, gutsandgrowth, assumes no responsibility for any use or operation of any method, product, instruction, concept or idea contained in the material herein or for any injury or damage to persons or property (whether products liability, negligence or otherwise) resulting from such use or operation. These blog posts are for educational purposes only. Specific dosing of medications (along with potential adverse effects) should be confirmed by prescribing physician. Because of rapid advances in the medical sciences, the gutsandgrowth blog cautions that independent verification should be made of diagnosis and drug dosages. The reader is solely responsible for the conduct of any suggested test or procedure. This content is not a substitute for medical advice, diagnosis or treatment provided by a qualified healthcare provider. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a condition
From NPR: COVID-19 Tests That Are Supposed To Be Free Can Ring Up Surprising Charge
An excerpt:
This reality means some medical providers… must rule out other respiratory diseases before ordering a COVID-19 test, leaving some patients with a difficult choice. Do they seek medical attention and risk a high medical bill? Or do they forgo care altogether?
A second hole in these federal protections may leave patients holding the bill for their COVID-19 test. The law prohibits insurers from charging patients for testing, but it does not block medical providers from doing so. If an insurer does not cover the total amount charged by a provider, the patient may get balance-billed, or slapped with a surprise charge.

From USAToday:


Related blog post:‘Quietly’ Testing Famotidine for COVID-19

From NY Times:

Elevated bilirubin in newborns with Down syndrome has been previously reported but the frequency has not been well-described. A recent retrospective report (TM Bahr J Pediatr 2020; 219; 140-5) compared 357 neonates with Down syndrome to 377,368 controls.
Key findings:
- Compared with control subjects, neonates with Down syndrome had 4.7 times the risk of having an initial total serum bilirubin exceeding the 95th percentile (23.5% vs 5.0%), 8.9 times the need for phototherapy (62.2% vs 7.0%) and 3.6 times the readmission rate for jaundice (17.4 vs 4.8 per 1000 live births).
The authors note that the basis for the increased risk of hyperbilirubinemia may be early hemolysis related to “neocytolysis” which is due to destruction of RBCs following a change from low to high oxygen exposure. Other factors could include slower bilirubin conjugation/elimination and poor feeding.
My take: This study indicates that infants with Down syndrome have a substantial risk of hyperbilirubinemia. And, while you are checking a bilirubin, it is worthwhile to obtain a direct bilirubin as cholestasis is increased in infants with Down syndrome too; the latter is often transient and/or associated with other organ involvement.
Related blog post: Neonatal cholestasis and Down syndrome

Island Ford Nat’l Recreation Area/Chattahoochee River, Sandy Springs
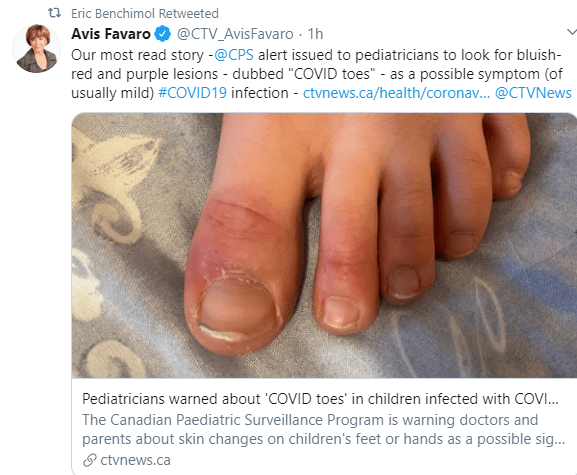
USA Today (4/27/20): Doctors find more cases of ‘COVID toes’ in dermatological registry. Here’s what they learned
An excerpt:
Dr. Esther Freeman, director of Massachusetts General Hospital Global Health Dermatology and member of the AAD task force on COVID-19, said COVID toes are pinkish-reddish “pernio-like lesions” that can turn purple over time…
While experts can’t confirm why COVID toes appear, they have some educated guesses. One could be inflammation in the toes’ tissue… Another hypothesis is inflammation of the blood vessel wall, medically known as vasculitis. And finally, … it is possible COVID toes could be caused by small blood clots that form inside the blood vessel…
COVID toes have appeared in some cases of asymptomatic patients. The majority of the toe cases manifested simultaneously or after more common COVID-19 symptoms, rather than before.
My take: During this pandemic, I need to look at my patient’s feet.
A recent report (JR Zucker et al. NEJM 2020; 382: 1009-17) highlights an outbreak of a vaccine-preventable disease, measles. Measles is much more contagious than the recent coronavirus; this is one reason why a vaccine is so crucial.
In total, there were 649 cases confirmed –most of the cases were in a close-knit community in Brooklyn, NY. 86% of the cases with a known vaccination history occurred in those who were unvaccinated. 49 required hospitalization. The cost to the Department of Health was $8.4 million.
My take: The health consequences and cost of not preventing measles is staggering -though being eclipsed by the coronavirus pandemic. The toll in Europe has been much higher. Worldwide more than 140,000 died from measles in 2018.
Related blog posts:

From Georgia Department of Health: COVID-19 Status Report
It is important to understand that some data, particularly in the last 2 weeks, may not be reported yet.




Related blog post (April 24): Why Georgia Isn’t Ready to Reopen
Yesterday, I received two emails (first from Steven Liu) about an article in Science and today I’ve already seen this article is referenced in a CNN report:
New York Clinical Trial Quietly Tests Heartburn Remedy Against Coronavirus
Key points:
- In China, a review of ~6000 patients suggested lower mortality in those taking famotidine (not statistically significant)
- Famotidine may interfere with viral replication protease in the coronavirus based on computer modeling
- A randomized trial with IV famotidine (large quantities are not available) is underway in New York using 9 times the dose used for heartburn.
- The article notes that increased heart problems are common in those with reduced renal function
- “We still don’t know if it will work or not”
My take: Famotidine may be a hot commodity –at least until studies are completed. Based on experience with hydroxychloroquine, some of our patients may need to look for alternative acid blockers.
Related blog posts:
- COVID-19 Projections -IHME Data IHME Link: IHME Website for COVID-19 This post details the projected needs (ventilators, ICU beds) and projected mortality. Currently, peak of this pandemic in U.S. is anticipated to be April 16th.
- How to Do a Colonoscopic Polypectomy and U.S. COVID-19 Tracker NPR: Map: Tracking The Spread Of The Coronavirus In The U.S This tracker details the pandemic in every state.
- How to Protect Healthcare Workers from COVID-19 -Lessons from Hong Kong and Singapore Atul Gawande has a very pertinent article in the New Yorker: Keeping the Coronavirus from Infecting Health-Care Workers
- What is the Current Standard of Care for PPE and Endoscopy Cases? Link to manuscript: COVID-19 in Endoscopy: Time to do more?
- Bill Gates: What We Need to Do Now for COVID-19, False-negative testing & Article Describing 3 Stages of Infection From NY Times: If You Have Coronavirus Symptoms, Assume You Have the Illness, Even if You Test Negative Bill Gates: Here’s how to make up for lost time on covid-19 & article describing 3 stages of infection: COVD-19 Illness in Native and Immunosuppressed States: A Clinical-Therapeutic Staging Proposal
- Allocating Scarce Resources During COVID-19 Pandemic Links CDC Link: Testing for COVID-19 Full Link NEJM 2020 (Ezekial J Emmanuel et al): Fair Allocation of Scarce Medical Resources in the Time of Covid-19. This post also displays some data on sensitivity/specificity of testing
- Iron Injectables Links Financial Times: Coronavirus tracked: the latest figures as the pandemic spreads | Free to read & from Johns Hopkins: COVID19 Caseload & Outcomes Worldwide
- COVID-19: Veneto vs. Lombardy and Georgia’s Part of this Pandemic Link: Harvard Business Review: Lessons from Italy’s Response to Coronavirus & Georgia DPH: COVID-19 Daily Status Report
- “Crushing It” Two More Pediatric Hepatitis C studies Full link from NY Times: How Long Will Coronavirus Live on Surfaces or in the Air Around You? and blog post shows how to properly place PPE
- Ethical Dilemmas and Digestive Symptoms –Common with COVID-19 Full link: NEJM: Facing Covid-19 in Italy — Ethics, Logistics, and Therapeutics on the Epidemic’s Front Line & digestive symptoms ACG: Full Link: ACG Media Statement
- More Advice on Coronavirus for Pediatric GIs: NASPGHAN and CCFA CCFA Guidance for Pediatric Caregivers and Patients —Updates on COVID-19 and IBD
- Autoimmune Hepatitis Outcomes, Grand Rounds on Splenomegaly, Hydroxychloroquine for SARS-CoV-2 & Zantac Warning
- Liver Shorts and COVID-19 Screenshots This post includes Fauci donuts, AJG reference on COVID-19 digestive symptoms, and technology to sterilized used PPE
- New: NEJM link to video demonstrating need for PPE during intubation -see picture at bottom of post. Fluorescent Spray During Intubation and at the bottom -there is an image showing how hydroxychloroquine and azithromycin could increase risk for life-threatening arrhythmias
A recent study (G D’Haens, O Kelly, R Battat et al. Gastroenterol 2020; 158: 515-26,editorial 463) describes the development and validation of a blood test panel to assess Crohn’s disease (CD) endoscopic activity level. The authors evaluated a blood test which measured 13 proteins in the blood using samples from 278 patients. Then there were two validation cohorts:
- 116 biologic-naive CD patients -cohort 1
- 195 biologic-exposed CD patients -cohort 2
The blood tests were used to develop an endoscopic healing index (EHI) score (0-100). Higher scores indicate greater disease activity.
Key findings:
- EHI values below 20 identified remission with a sensitivity of 97.1% and 83.2% in cohorts 1 & 2 respectively; specificity was 69% and 37% respectively.
- EHI values below 50 points identified patients with highest specificity of 100% and 88% in cohorts 1 and 2 respectively.
- EHI AUROC (area under the receiver operating characteristic curve) did not differ significantly from that of fecal calprotectin and were higher than measurement of serum CRP (in cohort 1 but not cohort 2).
The editorial notes that the EHI performed much better in younger, biologically-naive patients and that the EHI could potentially be incorporated into a treat-to-target strategy which would potentially entail followup endoscopy in those with EHI >50.
My take: While the stool calprotectin has some logistical barriers in many patients, the EHI is likely a much more expensive test and needs further validation. For now, the combination of CRP and calprotectin are the best noninvasive biomarkers to assess CD activity.
Briefly noted: Vedolizumab-Induced Pulmonary Toxicity -Case report of a patient with ulcerative colitis who developed interstitial lung disease (Gastroenterol 2020; 158: 478-9).
Related blog posts:


























