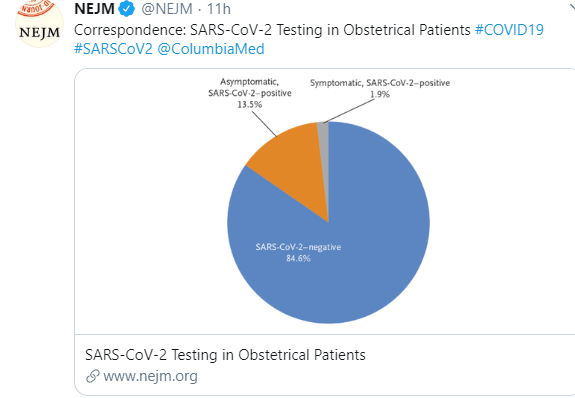
A study in Nature suggests that more than 40% of SARS-CoV-2 infections (COVID-19 viral infections) are spread in the presymptomatic stage: Temporal dynamics in viral shedding andtransmissibility of COVID-19 (Thanks to Steven Liu for this reference).
An excerpt:
We report temporal patterns of viral shedding in 94 patients with laboratory-confirmed COVID-19 and modeled COVID-19 infectiousness profiles from a separate sample of 77 infector–infectee transmission pairs. We observed the highest viral load in throat swabs at the time of symptom onset, and inferred that infectiousness peaked on or before symptom onset. We estimated that 44% (95% confidence interval, 25–69%) of secondary cases were infected during the index cases’ presymptomatic stage, in settings with substantial household clustering, active case finding and quarantine outside the home. Disease control measures should be adjusted to account for probable substantial presymptomatic transmission.
——————————-
A recent retrospective multi-center study (MR Nicholson et al. Clin Gastroenterol Hepatol 2020; 18: 612-9) provides data on fecal microbiota transplantation (FMT) for Clostridium difficile infection (CDI). Congratulations to one of my partners, Jeffery Lewis, who is one of the coauthors. This paper’s abstract is noted in a separate blog: Large Study Show FMT Efficacy/Safety in Children.
Though this is a pediatric study, the authors included patients up to 23 years. 335 of the patients had followup for at least 2 months following FMT.
Key findings:
- 81% of patients had a successful outcome after a single FMT and 86.6% after single or repeated FMT
- Higher success rates were associated with fresh donor stool (OR 2.66), FMT via colonoscopy (OR 2.41), and with not having a feeding tube (OR 2.08)
- Though not reaching statistical significance, patients with inflammatory bowel disease had a high failure rate of 23% (26/111). Short bowel syndrome patients had a 50% failure rate (5/10), solid organ transplant recipients had a 56% failure rate (5/9), and patients with feeding tubes had a 32% failure rate (21/65).
- Seventeen patients (4.7%) had a severe adverse event during the 3-month follow-up period, including 10 hospitalizations; however, the majority were unrelated to FMT. Specific adverse reactions that were related or may have been included aspiration pneumonia on day of procedure (n=1), IBD flare/colectomy (n=5), and vomiting/dehydration (n=1)
- Common adverse reactions included diarrhea, abdominal pain, and bloating. (These symptoms have been reported in up to 70% of adults following FMT.)
The authors note that a prior systematic review had indicated that delivery of FMT via colonoscopy was more successful in adults (95% vs 88%), though there are some additional risks with colonoscopy.
It is worth considering that the failure rate in some patients could be due to misdiagnosis, particularly in certain populations like patients with IBD and or organ transplant recipients. In these populations, PCR assays may result in false-positive diagnosis and should be confirmed with an ELISA assay. While eradication of CDI with FMT improves clinical symptoms and reduces the use of antibiotics the true benefit and risks will not be known for a long time. Does FMT increase or reduce the risk of downstream infections, autoimmune disease, and metabolic syndrome?
My take: Many of the concerns with FMT can only be adequately addressed with prospective studies (with strict definitions of CDI) and longer followup.
Related blog posts:
- FMT in the “Real World”
- Clostridium difficile/Fecal Microbiota Transplantation Video
- Something New with FMT
- Fecal Transplantation: “Frozen is as Good as Fresh” | gutsandgrowth
- Rejected! Most Stool is Not Good Enough for FMT | gutsandgrowth
- 4 points for C diff in Inflammatory Bowel Disease
- Clostridium difficile Infection in Inflammatory Bowel Disease: Expert Updates | gutsandgrowth
- Cost Effective Fecal Transplantation
- Keeping Up with Clostridium Difficile
- Overdiagnosis of Clostridium difficile with PCR Assays | gutsandgrowth
- Keeping Up with Clostridium Difficile | gutsandgrowth
- What’s the best medical therapy for Clostridium difficile? | gutsandgrowth
- Consensus Guidelines on FMT | gutsandgrowth